The Substrate Claim Status Agent is an AI-powered system that automates accounts receivable follow-up by checking claim status across 3,500+ payers using EDI, payer portals, direct APIs, and multiple clearinghouses. It requires no code changes to your practice management system and it replaces the manual process of logging into portals, calling payers, and interpreting 276/277 responses by using learned strategies that improve with every claim processed.
The healthcare world’s default tool for this is the 276/277 EDI transaction; providers can use these (via their clearinghouse) to check the latest status of a claim. But the 276/277 transaction by itself has a few problems:
- Every input you use must be perfect: the payer ID, NPI, member ID format etc. Get one of these wrong, and you don’t get a response
- Even when your inputs are right, the quality and depth of data you get can be tough. Sometimes all you get is an acknowledgement that the payer knows about the claim, but no actual detail about what’s wrong with it.
- Even if the first two go right, only ~500 payers support the 276/277 transaction. Compare this to ~1200 payers for eligibility, and ~2800 payers for claim submission/ERAs.
Bringing this altogether, failed claim statuses lead to lack of trust in the tool, and result in human billers stepping in to manually status a claim. This costs every single fee-for-service healthcare provider in the US time and money every single day. Patients pay more as a result.
The Substrate Claim Status Agent handles this automatically. When you submit a claim for status lookup, the Substrate Claim Status Agent doesn't just try once and give up. It works through recovery strategies based on what's failed before; for this payer, for this practice, for claims just like this one. It intelligently tries to get the richest claim status response back, and push it directly into your practice management system, with no code required.
How it works
The Substrate Claim Status Agent operates on three principles:
- Try the smart thing first. Before making any request, the Substrate Claim Status Agent checks what's worked for similar claims. If billing NPI succeeded for Cigna claims last week, it tries billing NPI first, not rendering NPI.
- When something fails, understand why, and iterate based on that failure. Different errors mean different things. "Entity not found" might suggest an NPI or tax ID issue. “Unable to respond” suggests that the payer is down and we should retry. The Substrate Claim Status Agent adapts based on these signals .
- Learn from every success. When a combination works, the Substrate Claim Status Agent remembers it via a concept we called “Learned Strategies”. This knowledge compounds over time - new claims benefit from everything the Substrate Claim Status Agent has learned across the millions of claims it’s already seen.
What the Substrate Claim Status Agent tries
The Substrate Claim Status Agent uses a classic sub agent architecture to explore a broad set of valid parameters across a broad set of routes:
Parameters include
- Practice identifiers: Tax IDs vs billing vs. rendering vs. facility NPIs
- Payers: different payer names and payer clearinghouse IDs
- Demographics: Different combinations of patient and subscriber names, gender etc
- Input combinations: Different payers require different inputs; some require submitted charges, others require subscriber info, etc
A simplified view of the overall Substrate Claim Status Agent flow:
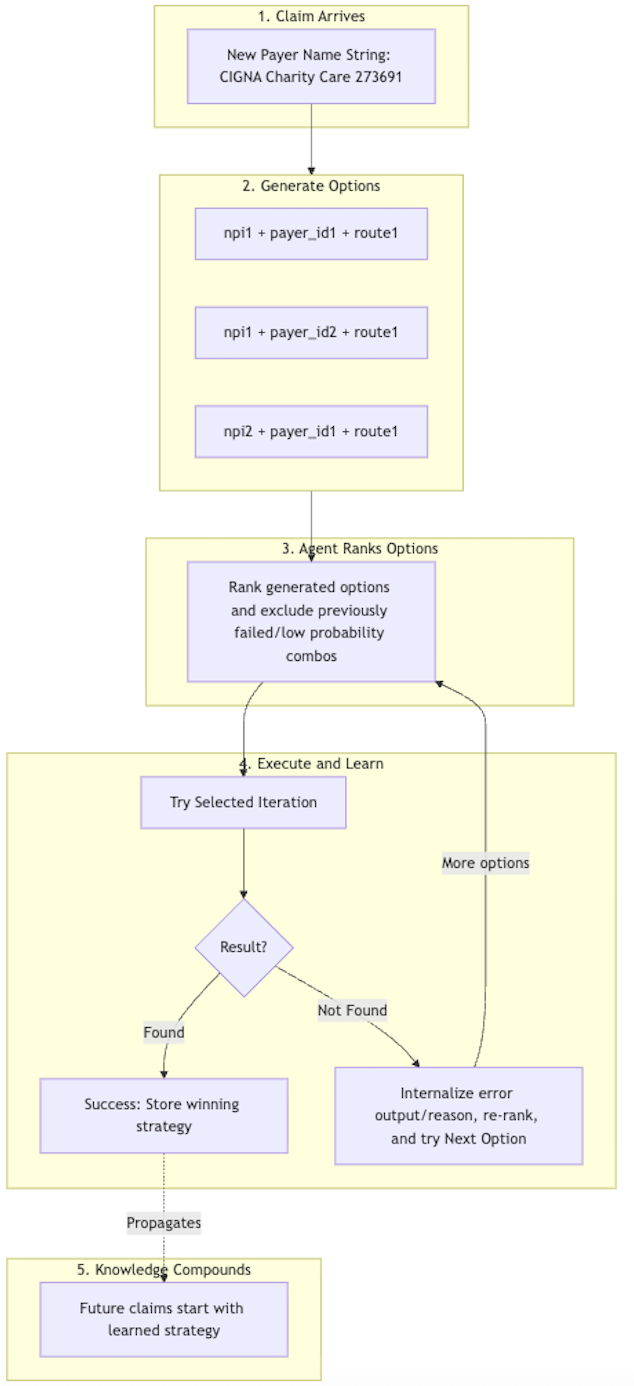
Over time the Substrate Claim Status Agent self enriches its own context, in addition to context we provide about different payers, parameters and routes. This might include live data about payer downtime, payer hours of operation, payer recommendations about required vs. recommended inputs, and more.
Options
The suite of options is quite broad and interacts combinatorially with routes. Options include anything you can change on a claim status submission, in service of retrieving the richest actionable response quickest. These include (non exhaustive list)
- Patient Demographics; eg some payers require gender to be submitted in the EDI route. Others might require a middle name be included in the portal
- Organization identifiers; some payers require the rendering NPI to be submitted, others require the billing NPI. Still others require you to submit an NPI along with an EIN.
- Encounter details: some payers require a charge amount to be submitted, others require a patient control number. Payer systems even vary by state in some cases.
- Payer specific nuances: different routes have different SLAs; some EDI endpoints are down during the evenings and some portals have lower response rates on weekends during weekends
The claim status Substrate Claim Status Agent is continually learning and building profiles of each payer so that for each claim status request, its routing optimally for the most actionable response.
Multi-route support
The Substrate Claim Status Agent doesn't rely on a single lookup method. It can:
- Hit EDI endpoints for payers that support 276/277
- Utilize multiple clearinghouses when one clearinghouse is down or when a payer favors another.
- Query payor portals via browser Substrate Claim Status Agent where available (or where the data is better)
- Use direct APIs for payers that support those.
- Fall back gracefully when one route is down
Results from all sources are normalized into a single, unified format and pushed directly into your practice management system, data lake, or system of record. We manage differences between different payers and routes, normalizing them into a format customized for your system of record and practice. This means your queues and worklists can automatically be updated daily based on the latest information about your outstanding A/R.
Importantly, we’ve built all these in a way that’s agnostic to the system of record you use - so trying it doesn't require you to spend expensive engineering resources, or to switch your RCM or PM system. You can even start with spreadsheets.
Who this is for
Almost every fee-for-service healthcare provider in the US faces a variant of this problem. The most sophisticated ones already have an agentic solution in place for handling claim status (if this is you, we want to learn from you).
For everyone else, your AR teams are wasting anywhere from 3 minutes per claim logging in, to 45 minutes on the phone waiting for a payer rep. If your teams spend any time on AR follow up, the Substrate Claim Status Agent will give them superpowers.
Learn more here, or book a demo here to learn more.
Frequently Asked Questions (FAQs)
What is an AI claim status agent?
An AI claim status agent is software that helps billers check the status of healthcare claims with insurance payers. This replaces the manual process of logging into payer portals, calling payer phone lines, or submitting 276/277 EDI transactions one at a time. The Substrate Claim Status Agent, built by Substrate AI, goes further: it uses a multi-route architecture that checks claim status across EDI endpoints, payer web portals, direct APIs, and multiple clearinghouses simultaneously, then pushes a normalized result directly into your practice management system. Unlike simple status-check tools that try once and stop, Substrate's agent uses learned strategies, including retry logic built from millions of prior claims, to automatically recover from failed lookups by varying parameters like NPI type, payer ID, member ID format, and demographic inputs until it gets the richest actionable response. The result is hands-free AR follow-up: your billing team gets updated claim statuses in their worklists every day without touching a portal or picking up a phone.
How does automated claim status work with payers that don't support 276/277?
Only about 500 payers in the U.S. support the 276/277 EDI claim status transaction. This is far fewer than the roughly 1,200 that support eligibility checks or the 2,800+ that accept electronic claim submissions. This gap is one of the biggest pain points in revenue cycle management, because it forces billing teams to fall back on manual methods for a large portion of their AR. The Substrate Claim Status Agent solves this by operating across multiple routes, not just EDI. For payers that don't support 276/277, Substrate's agent can query payer web portals using browser-based automation, connect through direct APIs where available, and route through alternative clearinghouses when a primary clearinghouse lacks connectivity to a given payer. Substrate currently supports over 3,500 payers across these combined routes. The agent selects the optimal route for each payer automatically. It accounts for historical success rates, payer downtime windows, and which input combinations (billing NPI vs. rendering NPI, with or without submitted charges, etc.) have worked for that specific payer in the past. All results, regardless of which route produced them, are normalized into a single unified format before being pushed into your system of record.
Can AI agents log into payer portals to check claim status?
Yes. The Substrate Claim Status Agent has a multi-agent architecture, and uses browser agents to log into payer portals and retrieve claim status information when portal access provides richer or more reliable data than EDI. This is particularly valuable for payers where the 276/277 response is limited; sometimes returning only an acknowledgement that the payer received the claim, with no detail about processing status, denial reasons, or expected payment timelines. Portal lookups often surface more granular information, such as specific denial codes, pending documentation requests, or adjudication timelines, that the EDI response omits. Substrate manages portal credentials, handles multi-factor authentication flows, adapts to portal UI changes, and respects payer rate limits and hours of operation. The agent treats portal access as one route among several. If a portal is down or rate-limited, it falls back to EDI or direct API routes automatically. This multi-route approach means your claims don't get stuck waiting for a single method to come back online.
How much time does automated AR follow-up save per claim?
Manual claim status follow-up typically takes between up to 18 minutes per claim ((according to the CAQH Index). This involves logging in, navigating to the right screen, entering claim details, interpreting the result, and updating the practice management system. Phone-based follow-up is far worse, as hold times alone average 20 to 45 minutes per call, according to industry surveys, and a single call may only resolve one or two claims. According to the 2024 CAQH Index, manual and partially electronic methods still accounting for a meaningful share of all claim status transactions. The Substrate Claim Status Agent reduces the human time per claim to near zero for routine status checks. Claims are submitted to Substrate in bulk, the agent processes them autonomously; retrying with different parameters and routes as needed, and pushes the results directly into your practice management system or data warehouse. Your AR team's time shifts from checking statuses to acting on them: working denials, filing appeals, and resolving the claims that actually need human judgment. For a practice processing thousands of claims per month, this typically translates to dozens of recovered staff hours per week.
Does Substrate work with my EHR / practice management system?
Yes. The Substrate Claim Status Agent is designed to be system-agnostic. It integrates with your existing EHR, practice management system, or billing platform without requiring you to switch systems or invest in custom engineering. Substrate pushes normalized claim status results directly into your system of record, so your worklists, aging reports, and AR queues update automatically based on the latest payer responses. Substrate has been deployed across a range of practice management systems and EHRs used by healthcare providers, billing companies, and healthcare networks. If your team currently works from spreadsheets, Substrate can start there too; you don't need a sophisticated technical setup to begin. Integration typically takes days, not months, and does not require changes to your existing EDI or clearinghouse relationships.
How many payers does Substrate support?
The Substrate Claim Status Agent supports over 3,500 payers across its combined routes. This includes EDI (276/277), payer web portals, direct APIs, and multiple clearinghouses. For context, only about 500 payers support 276/277 EDI for claim status, approximately 1,200 support electronic eligibility verification, and roughly 2,800 support electronic claim submission and ERA. Substrate's multi-route architecture closes this coverage gap by reaching payers through whatever channel works best for that specific payer and claim type. The agent continuously builds payer-specific profiles that track which routes, input combinations, and timing produce the highest success rates, so coverage and data quality improve over time as the system processes more claims.
What's the difference between 276/277 EDI and an AI claim status agent?
The 276/277 is a HIPAA-mandated electronic transaction standard: you send a 276 request with claim details to a payer (typically through a clearinghouse), and the payer returns a 277 response with the claim's status. It's the industry's default electronic method for claim status inquiries, but it has significant limitations. First, every input must match exactly; payer ID, NPI, member ID format, date of service. A single mismatch returns no usable response. Second, many 277 responses contain minimal information, sometimes just confirming the payer received the claim without any detail about adjudication status, denial reasons, or expected payment dates. Third, only about 500 payers support the 276/277 transaction at all, leaving thousands of payers reachable only by portal or phone.
An AI claim status agent like Substrate's sits on top of 276/277 and extends it. When a 276/277 lookup fails, the Substrate Claim Status Agent doesn't stop. It analyzes the failure reason and retries with different parameters (e.g., switching from billing NPI to rendering NPI, adjusting the member ID format, or adding submitted charges). If EDI isn't the right route for a given payer, the agent automatically falls back to payer portal lookups, direct APIs, or alternative clearinghouses. It also learns from every interaction: successful parameter combinations are stored as learned strategies that benefit future claims to the same payer. The net effect is higher success rates, richer data, and coverage across 3,500+ payers instead of the roughly 500 that support 276/277 alone. And all of this is available without requiring your billing team to change their workflow or learn a new tool.


